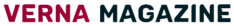There is a critical need to comprehend the connection between prior ailments and Coronavirus illness result.
Chronic obstructive pulmonary disease, cardiovascular disease, hypertension, and diabetes mellitus have all been linked to an increase in COVID-19 severity in previous studies. Patient characteristics such as older age and male sex are linked to an increased risk of COVID-19 mortality in addition to these comorbidities.
One review, distributed in JAMIA Open, looked to assess patient socioeconomics and comorbidities as hazard factors for extreme Coronavirus. However, the investigators wanted to carry out their analyses in Indiana, specifically in the Midwest of the United States.
The study’s authors wrote, “The Midwest has some of the highest prevalence of comorbidities, specifically hypertension, COPD, and diabetes.” To better understand the connection between comorbidities and COVID-19 outcomes in this region, it is necessary to analyze a large, comprehensive cohort of Midwest patients.
The researchers obtained electronic health record (EHR) data from 776936 COVID-19 patients and 1362545 COVID-19 patients by making use of the COVID-19 Research Data Commons (CoRDaCo). The clinical data warehouses of Indiana University Health and Eskenazi Health, in addition to the Indiana Health Information Exchange, comprised the CoRDaCo data.
Patient information was gathered between January 1, 2018 and May 5, 2021 for the study. The positive COVID-19 cases were confirmed by laboratory testing, whereas the negative controls had at least one Indiana Network for Patient Care encounter and one negative COVID-19 test result between 2018 and 2019.
The 12 comorbidities that were looked at in the study were chosen because they are common in Indiana and have been linked to COVID-19 severity. The US Census Bureau provided information regarding the population of the county as well as the income per capita. The purpose of the statistical analysis carried out by the researchers was to ascertain whether or not there was a correlation between the severity of COVID-19 and various clinical and demographic variables. Utilizing prescient examination, they assessed the prescient force of CoRDaCo EHR information in deciding Coronavirus sickness seriousness.
The researchers found that 4.76 percent of COVID-19 patients had type 2 diabetes, 3.49 percent had cardiovascular disease, and 3.49 percent had chronic obstructive pulmonary disease. Patients with these co-morbidities had an increased risk of admission to the intensive care unit (ICU) by 10.23 percent, 14.33 percent, and 11.11 percent, respectively. All of these rates were significantly higher than the 1.94 percent ICU admission rate for the entire COVID-19 patient population.
In addition, the COVID-19 patient population as a whole had lower mortality rates than those with cardiovascular disease, type 2 diabetes, and chronic obstructive pulmonary disease.
Black COVID-19 patients in Indiana experienced more adverse outcomes than White patients when disease severity was categorized by demographics. In the United States, COVID-19 mortality and morbidity disparities are consistent with these findings. Potential wellbeing abberations in Indiana demonstrated contrasts in medical services openness, as well as portrayal in CoRDaCo.
According to the study’s authors, “ICU death rate was also higher for COVID-19 patients with comorbidities than for controls with that comorbidity.” “Overall, COVID-19 patients with any of our considered comorbidities had higher death rates than controls (i.e., patients without COVID-19) with that comorbidity,” the authors wrote.
The researchers came to the conclusion that the CoRDaCo EHR data are adequate for estimating a patient’s risk of COVID-19 infection and determining whether a COVID-19 patient will require ICU admission.